Dear Friends
I do not have TV at my house. When the earthquake hit Haiti I only heard stories and my imagination made the pictures for me. I heard of incredible destruction and death, of a lost child finding his way to an orphanage and being turned away. The orphanage had fallen and they could not take care of the children they had. The image of a parent less child wandering the streets alone, that is when I decided I was going to Haiti. The rest is history. Laura and I joined together, she took on organizing the medical mission and I took on the children, we decided to find an orphanage to sponsor while working at the Hopital. Before we left for Haiti we began planning a benefit music festival for the children. We found our orphanage and chose it because it is a safe and loving home. Today I called Charlucie (Lucie) Jaboin the president of the Reveil Matinal Orphanage Foundation, she is Haitian and lives in New York City. This is the girls orphanage in Port au Prince we wrote about in a previous blog. It is the home of 20 girls age 3 to 12. Their dream is to move to a larger place that will be able to have boys, and will be located within walking distance of the Hopital Adventiste d'Haiti. Today I told Lucie that we want to help her realize this dream. Charlie MD and I are going to be interviewed on our local public radio station KZYX/KZYZ 91.5 and 90.7 on Wednesday June 2 from 9 to 10 am. For people out of Mendocino County you can stream the show on the web at kzyx.org. We are going to call the orphanage and the girls are going to sing for us.
While working at the Hopital I came to realize a deeper value of song. Groups of people would break out in song throughout the day. A person may have lost everything and they still sing. The singing is beautiful, healing and full of love. The music gave us a sense of peace and true beauty.
Please Save the date for our benefit: Hearts Helping Haiti, Saturday, August 21, 12 to 7 pm, family fun, music festival, at the Nelson Ranch, south of Ukiah. Please volunteer to help we will need 100 people that day. We are having 2 slide shows/receptions on June 17 and 18 as a kick off for the benefit.
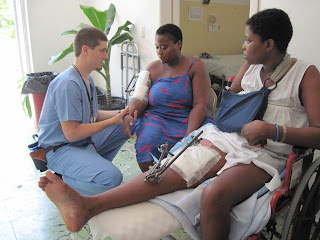
The following story is about Adnise, the 22 year old woman who walked with David and Melanie for the first time in her life.
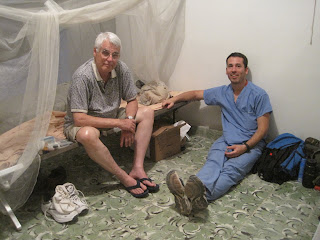
Pictures: The Girls of Reveil Matinal Orphanage, Ukaih Team at work in the ER at UVMC Skip in the middle is in Haiti now and our wonderful supportive Hospital President Terry Burns toward the right, David and the shoes for Adnise.
Words by David our Physical Therapist
I am not going to be so arrogant as to say that Adnise has never owned any shoes. While likely she hasn’t it is always possible. I can assure you that none of them have been adequate to actually fit her bilaterally clubbed feet. This is a project that we have been working on for the last week. Once I saw how good she was doing walking I enlisted the help of one of our great handymen. After I introduced him to this young woman, he wanted to make some good shoes for her as badly as I did. He took wooden reinforced shoes and cut them down to her size and rounded the edges. We then spent a good chunk of the afternoon sewing straps on. Once we had them all fixed up we took them down and gave them to her. She was experiencing some muscle cramps when we arrived which definitely dissipated some of the excitement of the moment. After a little soft tissue work on her feet she was smiling and ready to be up and trying out her new shoes. She was able to walk much better without the pressure of the hard tile floor on her little feet. She continues to complain of the weight of her braces which are actually very light, but when you haven’t walked in your entire life, everything seems heavy.
Everyday we try to make as much of a difference as we can, sometimes it is the little things that mean the most. Building relationships is as important as anything else that we are doing here. It is an opportunity for us to step back and realize that we
don’t have a list of things to accomplish, we are here to reach out to people in whatever way we can.